
Not all acne is created equal and if your breakouts aren’t getting better, it might be because you’re treating the wrong kind.
At Lucid Dermatology, we see this every week. Patients come in frustrated after months or years of breakouts that just won’t go away. Many have tried every trending product under the sun, but what they really needed was a proper diagnosis. That’s because what looks like acne may not actually be acne. In fact, one of the most common culprits we see misdiagnosed is fungal acne.
Fungal Acne vs Bacterial Acne: Let’s break down the difference between these two skin conditions and explain what you need to know to finally clear your skin.
Fungal acne isn’t technically acne at all. The term refers to a condition called Malassezia folliculitis, caused by an overgrowth of yeast (a type of fungus) in the hair follicles. This yeast is normally present on the skin, but certain conditions like excess sweating, humidity, or occlusive skincare products can throw off the balance and cause inflammation.
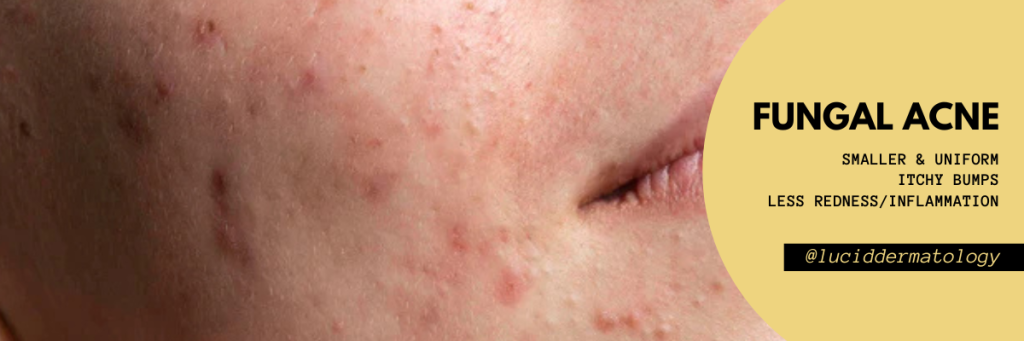
It typically appears in clusters, especially on the chest, back, shoulders, or forehead. It doesn’t respond to traditional acne treatments. In fact, products like salicylic acid, benzoyl peroxide, or even oral antibiotics can sometimes make things worse by further disrupting the skin microbiome.
This is the acne most people are familiar with, technically known as acne vulgaris. It’s caused when dead skin cells and excess oil clog the pores, creating the perfect environment for bacteria (usually Cutibacterium acnes) to multiply. That leads to inflammation and visible breakouts.
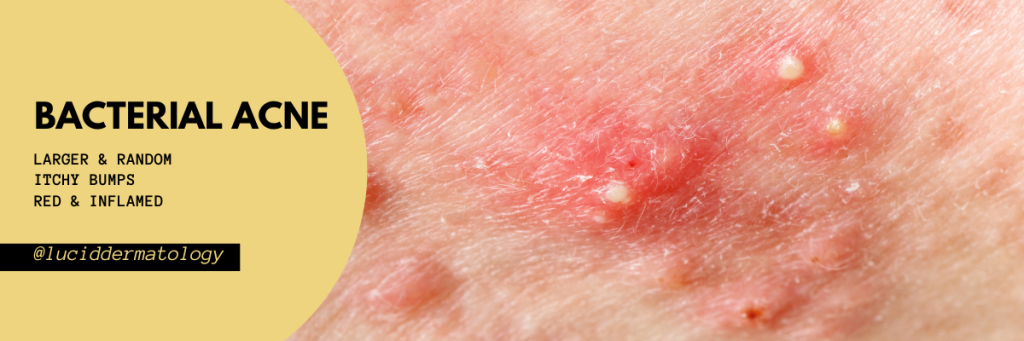
It often presents as a mix of whiteheads, blackheads, and inflamed lesions (papules, pustules, cysts). Breakouts may be painful or tender, found on the face, chest, or back, and they often respond—at least somewhat—to traditional acne treatments.
While many over-the-counter treatments can help with mild cases, moderate to severe bacterial acne often requires professional treatment. That might include prescription topicals, oral medications, or in-office therapies.
The symptoms may look similar but the treatments are very different. That’s why getting a clinical diagnosis is so important.
At your visit, we’ll review your full medical history, evaluate your current skincare routine, and examine the pattern of your breakouts. In some cases, we may perform a quick, painless diagnostic test to confirm the presence of yeast versus bacteria.
Once we know what we’re dealing with, we’ll create a plan designed to clear your skin, not just temporarily, but for the long term.
If you’ve been stuck in the cycle of trying new products every few weeks and seeing no progress, the real issue might be misidentification. Treating fungal acne like bacterial acne won’t work and vice versa. Our job is to help you stop guessing and start healing.
At Lucid Dermatology, we treat all types of acne with expert care, clear answers, and a plan that actually fits your skin.
Think your acne might not be acne? Schedule a consultation and let’s figure it out together.